3 common foot conditions – diagnosis and treatment
Having painful feet can be so debilitating. Here we take a look at 3 common foot conditions; which, although not life threatening, may seriously affect your wellbeing.
Morton’s Neuroma
A condition which affects the nerves in the foot involving thickening of the tissue around the nerve between the bases of the toes – most commonly between the 3rd and 4th toes.
Morton’s Neuroma is especially common in women as it’s often triggered by the wearing of tight or heeled shoes.
Usual symptoms can include sharp shooting and burning pain to the ball of the foot, and tingling and numbness of the toes with pain becoming worse on walking and weight bearing.
If you feel that you are suffering from these symptoms then we advise an assessment by a Podiatrist or your GP.
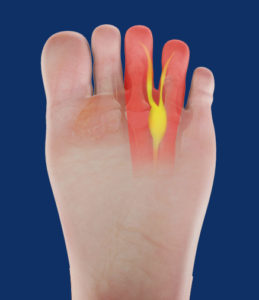
Morton’s Neuroma
Treatment for Morton’s Neuroma
The usual treatment advised for Morton’s Neuroma is a change of footwear, orthotics, analgesia or steroid injections. Weight loss is also commonly encouraged.
If after these initial treatments symptoms worsen or become more severe then your foot specialist may recommend surgery.
During surgery the foot specialist will increase the space around the nerve or even remove part of the affected nerve to minimise any future discomfort. Surgery is conducted under general and local anaesthesia and will take some weeks for a full recovery.
Read more on the consequences of wearing high heeled shoes.
Ingrown toenail
An ingrown toenail develops when the corner or side of a toenail grows into the surrounding skin. The result is pain, redness, swelling and, sometimes, an infection. The condition is very common in both men and women and the big toe is more likely to be affected as that nail tends to be the thickest and strongest, and is likely to be the main victim of overcrowding in shoes.
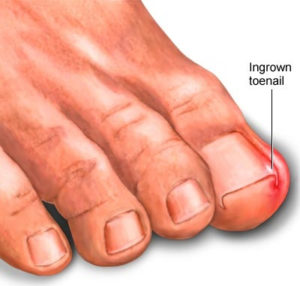
Ingrown Toenail
You can treat an ingrown toe nail at home by soaking the affected foot in warm water 3 – 4 times a day for a few days, making sure you wear wide comfortable shoes and taking an over the counter painkiller such as paracetamol or ibuprofen to ease the pain.
If treatment at home is not helping, your toe is still very painful and swollen with pus coming out of it, you develop a high temperature or you have diabetes then you should make an appointment with your GP for an assessment.
A GP can give you antibiotics and may refer you to a foot specialist.
Treatment from a foot specialist
A foot specialist (podiatrist) may offer further treatments, such as cutting away part of the nail or removing the whole nail.
You’ll have an injection of local anaesthetic to numb your toe when this is done.
Before surgery you can take paracetamol but not more than 2 at a time and no more than 8 in 24 hours. You will need to seek advice from your surgeon if you wish to take Ibuprofen.
If you are worried about the pain of the injection then you may wish to ask for Emla cream to be applied on the area as this will numb the skin.
If you are needle phobic then you may ask for special needles where the needle is concealed so you cannot see it piercing the skin.
Preventing ingrown toenails
To help stop ingrown toenails:
- do not cut your toenails too short
- cut straight across the nail, not the edges
- do not wear shoes that are too tight or do not fit properly
Pins and needles in feet
Temporary pins and needles occur when pressure cuts the blood supply to your nerves and stops them communicating with your brain. So if you suffer from pins and needles only while you are walking then it could be caused by pressure on your foot.
Causes of temporary pins and needles in the feet could be:
- shoes are too tight and pressing on your nerves
- the way you walk (your gait)
- Raynaud’s syndrome – where blood vessels spasm and stop the blood supply, usually when your body is cold or stressed (can last a few minutes or a few hours)
Check your shoes and gait for any pressure spots which may help with your symptoms. A physiotherapist will be able to check your gait and some gyms or specialist running shops will be able to provide an assessment too. An insole may be all you need to correct the way you walk.
Continuous pins and needles should be checked out by your GP as it could be a sign of an underlying health problem such as:
- Diabetes – this condition causes poor circulation and can affect the nerves in your feet
- Sciatica – something may be irritating or squeezing this nerve which runs from your back, through your hips and down to your feet.
Less common causes of pins and needles are alcohol abuse, malnutrition, exposure to toxic substances, as a result of an injury or infection and suffering a stroke.
It is important to meet with your GP if you have permanent pins and needles in your feet as they will be able to assess you for any treatment needed.
Read more about conditions such as plantar fasciitis and bunions.
Disclaimer
All content on Silversurfers.com is provided for general information only, and should not be treated at all as a substitute for the medical advice of your own doctor or any other health care professional. Silversurfers will not be responsible or liable for any diagnosis made by a user based on the content on www.silversurfers.com and we are also not liable for the content of any external websites or links from or to Silversurfers to any other websites. Please always consult your own doctor if you’re in any way concerned about any aspect of your health.
Melina - Assistant Editor
Latest posts by Melina - Assistant Editor (see all)
- Top tips for hay fever sufferers - April 14, 2024
- Paysan Breton Cream Cheese Breakfast Wraps - April 12, 2024
- 4 Homemade Sweet Treats for Easter - March 24, 2024
- Playground Memories - March 10, 2024
- The invasion of the duvet: the ’10-second bed’ - February 20, 2024